First, my humble thanks to everyone for the sympathetic Tap-Repeatedly response to my unexpected medical adventure(s). I continue to be warmed by your kind wishes and can happily report that I am healthy, active, and glad to be alive.
I can also report that I think I have finally solved the mystery of why I was bleeding in the first place. Sort of had to. None of the medical professionals I interacted with had any explanations to offer, so I became a detective on my own behalf. This is that story.
A Bit of Background
For those who may not be familiar with the entire medical drama, you can read about it here. For those who are familiar with it, the following will serve as a condensed reminder.
I am a muscular, if overweight, 61 year old male with controlled high blood pressure. My doctor has, for years, had me on fish oil, lisinopril (keeps my blood vessels from contracting), and low dose (81mg) aspirin. The only effect these pills have had on me is the desired one of lowering my blood pressure.
In October of 2011, I went into the hospital with a very mild chest pain and was prescribed, in addition to the drugs I was already taking, a drug which is supposed to further lower my blood pressure: metoprolol, a beta blocker that would slow my heart and expand my blood vessels.

Metoprolol
Six days later, after taking my daily doses of low dose aspirin, fish oil, lisinopril and metoprolol, I was taken to the emergency room with a massive lower gastrointestinal bleed (LGIB). Massive, used in this sense, refers to the loss of more than two units — a unit is just less than a pint — of blood. In three days, in episodes that resembled diarrhea, I needed six units of blood to replace what I expelled — roughly half the blood in my body.
On the fourth day, no longer bleeding, I was discharged from the hospital and told to restart all drugs except low dose aspirin. I was to restart the aspirin in a week.
Three days after restarting my aspirin, I was back in the hospital with a second massive LGIB. This time I lost seven units. The decision was made to take me off aspirin permanently.
As I mentioned, not one of the professionals attending me during these two bloody episodes had any explanation for why I was bleeding. Tests were performed, procedures were done, questions were asked. The results were all negative. While many things were ruled out, nothing remained as a possible cause. If all the results had been reduced to a gesture, it would have been a shrug.
Mulling it Over

Heparin
As my multiple hospital stays slid silently into memory, I found myself less and less satisfied with the idea that massive bleeding, especially in an old man like me, just happens. That seemed like a lazy excuse for an explanation. Nor was I satisfied with the idea that I had suddenly become allergic to aspirin after taking it for years without incident. I wasn’t even satisfied with my own theory that the clot-busting heparin (an anticoagulant I was given during the diagnosis of my heart condition) had somehow made me hypersensitive to the anticoagulant effects of aspirin.
I started researching, with an eye to their interactions, the drugs I had been taking and laid out in chart form the days on which I had been taking them. And, sure enough, the answer emerged.
It wasn’t the aspirin.
Or, to be more precise, it wasn’t the aspirin alone. The bleeding only occurred after several days of taking two drugs together. Taking either one alone produced no side effects. The chart revealed that, prior to the first bleed, I had been taking both aspirin and metoprolol for six days. After the first bleed, I was told to restart all drugs, except aspirin, and then restart the aspirin after a week. Within three days of taking the metoprolol and aspirin together, I was bleeding again. My bleeds were the result of a drug interaction which produced a rare severe side effect. Following my last hospital stay, I was taken off both aspirin and, eventually, metoprolol. Whew.
Try Asking Your Doctor
Since one can’t call or email a doctor in the USA in 2012, I wrote an actual physical letter — with an envelope and a stamp and a return address and everything — to the internist who originally prescribed the metoprolol for me. My intent was to let him know what metoprolol and aspirin are capable of when they get together. To date, there has been no response.
Drugs.com naively puts it this way:
Call [HA!] your doctor at once if you have any of these serious side effects [while taking metoprolol]: easy bruising, unusual bleeding (nose, mouth, vagina, or rectum)…
The [HA!] part I added. Writerly license. Sue me.
The list goes on at some length, but the only thing that caught my eye was the “unusual bleeding” part. Oddly enough, the package insert that came with my metoprolol prescription made no mention of bleeding, unusual or otherwise.
Drugs.com goes on to say:
In addition, beta-blockers (like metoprolol) may exert an antiplatelet effect, which may be additive with the effects of some salicylates (aspirin).
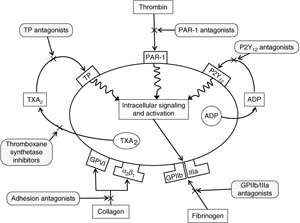
Platelet
Antiplatelet is one of the three types of anticoagulant. Aspirin is an antiplatelet. I was, without knowing it, taking a double shot of pharmaceuticals which prevented my blood from clotting. While taking one or the other was no problem for me, taking them together was like chugging a battery acid Big Gulp.
I did manage to reach the physician’s assistant who saw me during my first bleed and the nurse of a surgeon who had been called in to advise during my second bleed. The physician’s assistant, an eager young fellow, heard me out, thought it sounded provocative, and set off to do his own research on metoprolol. The nurse was surprised at the suggestion that there might be a adverse drug interaction with low dose aspirin and metoprolol because it’s common to prescribe them together to heart patients. I pointed out that the rarity of the effect could lead physicians to assume, based on the largely uneventful experience of their patients, that it never happens. As a food safety expert once told me, “Rare is not the same as never.”
I also groused a bit about one of the attending physicians calling my bleeding “inexplicable,” which, the nurse agreed, is not something you want to hear from a doctor. Unless, of course, the doctor is being played by Richard Carlson and he’s reacting to something bizarre in a 1950’s Jack Arnold science fiction film. Then it’s fine.
And there is more from Drugs.com:
Metoprolol may also increase aspirin absorption and/or plasma (blood) concentrations of salicylates (aspirin); however, the clinical significance of this effect is unknown.
I’d suggest the clinical significance of increasing the absorption of an anticoagulant and/or concentrating an anticoagulant in the blood might include spontaneous bleeding, but I’m just guessing here.
So THAT’S what Happened!
As far as I’m concerned, the mystery is solved. My particular body chemistry reacted badly to two commonly prescribed drugs that are commonly prescribed together. Not surprising that the folks keeping me alive didn’t have time to wonder about what might have been responsible for bringing me to the ICU.
Twice.
Rapid blood loss, no matter how often it happens, tends to crowd out contemplative curiosity.
The side effects also explained the progression of my bleeding episodes. Once in the hospital, the blood flow slowed and stopped because I was taken off all drugs upon admission. As the aspirin and metoprolol cleared (left) my system, their anticoagulant effects abated and I quit bleeding. Once I restarted my prescriptions, their anticoagulant effects returned and so did my bleeding. Simple.
For those with an interest in health care costs, some numbers:
Cost of drugs to get me into this mess: about $7 USD
Cost of hospitalization to get me though this mess: $65,000 USD
Benediction
Thanks again, dear Tappers, for your concern and sympathy. Your emotional support has meant more than you will ever know.
Now, let’s celebrate by playing something! DIY diagnosis
![]()
Tell MrLipid you’re glad he’s alive at mrlipid@tap-repeatedly.com.


Glad to hear you are out of the woods on this mrlipid. When I was younger I tended to put complete trust in doctors. Your stories and others like it (both my parents have had to be rushed to the hospital because of prescribed drug interacting in very, very bad ways) have made me much more questioning.
Call your doctor? Right. Call the office and leave a message for an overworked assistant who will eventually get back to you if you haven’t dropped dead in the meantime.
$65,000.00 for 13 pints of blood is 5,000.00 a pint. I wonder if I could sell my blood on eBay for say a 1,000 a pint and undercut the hospitals? Would the hospital give a discount for BYOB patients?
MrLipid, I still feel that you are lucky to be here today writing this conclusion up for us to mull over. Lucky and tough that is. Whew, what an amazingly bad ordeal you had to go through, not once but twice. Good detective work though, I’m quite surprised that not one medical expert put 2 and 2 together to connect the dots between the aspirin and metoprolol.
@Scout: Thanks. As for being trusting, I used to be pretty trusting, too. Now I find myself more, um, skeptical.
@lakerz1: I do feel lucky. And not as surprised as you might think that no one figured out what was happening.
First, who wants to admit that they are part of an enterprise that insists people take potentially lethal drugs? No one. So, assuming the drugs aren’t the problem, what is?
Second, it’s a standard prescription for heart patients and, as far as anyone knows, they aren’t all leaking blood.
Third, it’s such a low dose of aspirin it couldn’t possibly be a contributing factor.
Fourth, when someone who has been bleeding stops, there is nothing else to do for them. There is no treatment for folks who aren’t bleeding and no one bothers to ask why they were bleeding in the first place. Just wait ’til they stop and send them home.
Fifth, even if episodes of uncontrolled bleeding do happen, they happen so rarely that it hardly matters. Except, of course, to the person it happens to.
Sixth, since I was seen by two totally different emergency teams, I was, in effect, seen for the first time…twice. No continuity of care and no overlap of staff. I have no idea what, if anything, was shared between the teams.
I, too, used to put total trust in doctors. My own experiences – no where close to yours in any way, shape or form – have set my skeptical level to 11 and led to the conclusion that unlike TV writers would have you believe, modern-day doctors aren’t that far removed from simply casting chicken bones and reading tea leaves in their attempts to “cure” their patients. Although true chicken bone-casting practitioners aren’t throwing lethal drug combinations into the mix.
Glad you were able to figure out the true cause, Mr Lipid. Maybe you could bill your time and effort as an offset?
@Toger: My first exposures to emergency medicine left me impressed and dismayed. Impressed by the professionalism of the team(s) in handling my emergency needs and dismayed by the inability of the doctors to come to terms with the problem I presented them with.
Twice.
I felt like a essay question that no one could come up with plausible answer to. I think the doctors were glad when I quit bleeding because then I could be sent home, no answers required.
As for billing them, I fear I am only a civilian whose opinion carries no weight at all. 😉
My opinion may be subject to mistrust because I am a med student, so I will refrain from commenting on the replies to Mr.Lipid’s article. In any case, my primary concern with patient skepticism is not that they are skeptics in itself, it is their right and duty to be so, because doctors aren’t gods, and the patient should always be active in their healing. The main fear is that that distrust could lead people to trade medicine for literal reading of chicken bones and tea leaves.
But that’s not why I’m here, commenting. I’m here because, deciding to read what I believed was a gaming site (among other things, I know), I was linked to the article about your health problems. I’m not complaining, though, just keep reading.
I read my share of medical cases, and occasionally find cases written by the patient, which tend to be biased complaints and occasionally justified anger tantrums, or just pseudoscience endorsements. But I’m delaying myself, probably trying to sound more eloquent and more polite than I am. Bottom line: this was the best of such articles. It was gripping and objective, and funny, and every development was followed by informative notes on the working of the body or the drugs, which is quite a step up.
I really want there to be a blog about medical cases written like that from patient perspectives, and that not happening any time soon, I can only wish you get sick more often.
Kidding, kidding… or am I?
Just another thing, when I was twelve I had to take the same liquid they gave you before the colonoscopy, and I cringe just by being reminded of it. I gave up before I finished the first bottle, it was that awful (plus I was kid). So I can relate at least to that part.
@gervasium: Glad you found it of value. Flattered, even. And, that said, don’t really want to get sick more often. And I’m not kidding.
Pulling back a bit, I suspect most of the folks who treated me were surprised by the qualities you found appealing: I was both upbeat and cold blooded. Able to express enthusiasm and objectively discuss personal physiological issues. “Would it help if I bled? How much would you like?”
No illusions on this end about how things were supposed to play out. Which is an interesting place to stand when writing about things like undiagnosed uncontrolled bleeding.
I would offer you, a med student, this advice: Don’t sleepwalk through your rounds. People are depending on you. The standard treatment is usually, but not always, what’s needed. May, in rare cases, be potentially lethal. Outliers have a lot to teach you. Remember your oath.